Pain - it's your body shouting at you!
The way your body moves influences how it functions. The body is designed to cope with challenges and to adapt when things get tough. However if injury takes it by surprise, stress goes on for too long or work and hobbies push it beyond its comfort zone it can become overwhelmed and run out of ways to turn.
The end result is often pain and discomfort, whether it be sudden and dramatic or niggling and non specific. Pain is your body shouting at you that something's not right and it's not coping. Painkillers tell the body to shut up! Osteopaths actually listen and find a solution.
Helping the body to look after itself
The practice of osteopathy includes applying skilled soft tissue stretching/ balancing techniques and joint mobilisations and adjustments with the aim of restoring movement and function which has been lost. Osteopaths firmly believe that the body is very good at looking after itself when it is in the right condition to do it. We simply help provide that environment.
Osteopaths are best known for backs, but we can help with most problems that relate to muscle, tendon, joint, disc, nerve and ligament damage. These include, but are not restricted to:
- Low back problems – including sciatica, pain and stiffness, ‘wear and tear’, ‘trapped nerves’, disc injuries
- Head pain (some fancy advertising lawyer tells me I can’t say “headaches” so I have to let you figure what is meant by head pain!)
- Osteoarthritic joints – we can’t cure you, but we are successful at being able to substantially improve the symptoms associated with this condition
- Sports injuries – including ankle injuries, over-strains and over-training injuries
- Childhood aches and pains
- Neck pain – especially when it spreads into shoulder/arm/hand
- Tennis elbow (outside of elbow) and golfer's elbow (inside)
- Hip, knee and foot complaints
- Shoulder problems – especially rotator cuff and frozen shoulder problems
- Muscle and ligament injuries
What happens during a session?
Your story
First and foremost an osteopath will gather information. A detailed case history about your current and past symptoms, general health, accidents, operations, medications and lifestyle is a vital part of the problem solving. Even when you might think it's not relevant, we genuinely need and want to know the finer details.
The body is not neatly packaged in sections, as the anatomy books would have us believe. Your body is a whole - a single functioning unit - and every aspect of it is important with regards to the whole. Your story is important, so we make sure you have plenty of time to tell it.
Assessment
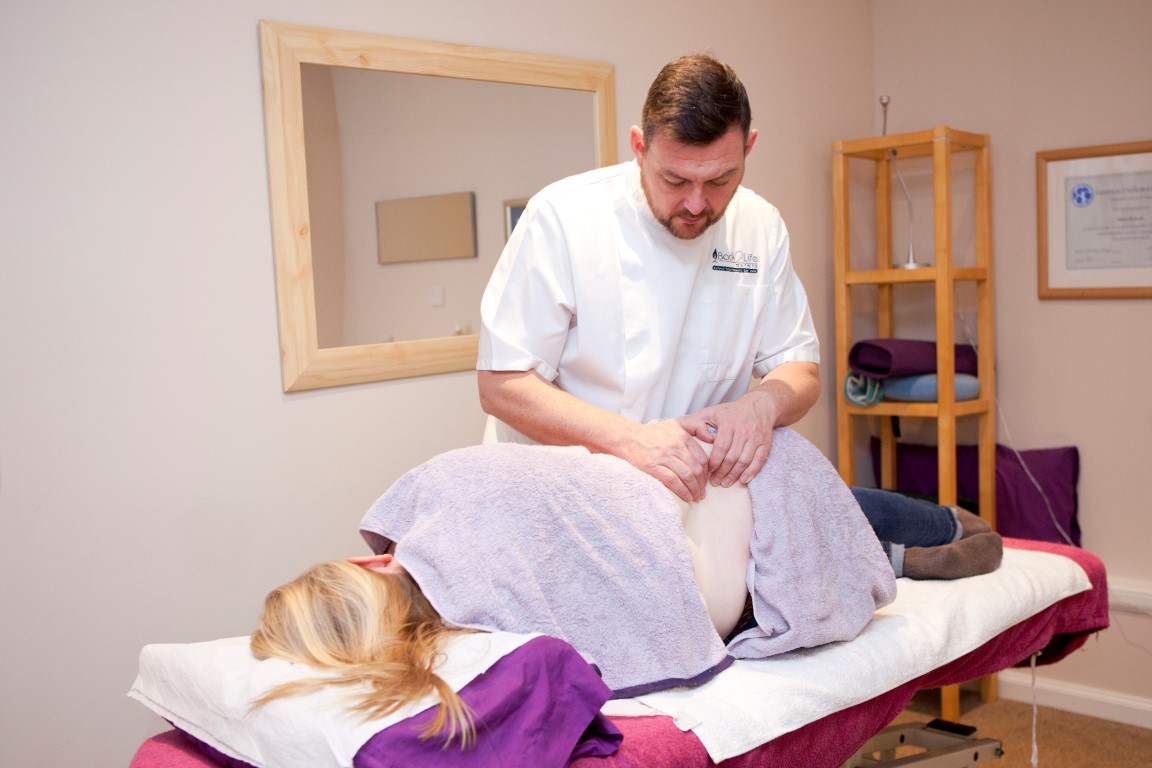
Next your osteopath will need to assess the function and mobility of the body in general and look for areas of excessive tension, weakness or inflammation. Patients are asked to undress to underwear to ensure the entire body is visible. We really do need to see you clearly in order to make a sound judgement about what's going on. Once this has been done blankets and towels are on hand if you'd rather have a bit of cover up.
First we'll ask you to go through a few basic movements while standing and then, with you lying down, we'll run through some passive mobility tests (where you try to relax and let us perform the movement) relevant to what we've put together from case history and examination so far. Not only are we assessing general movement and function of joints but also the tone of the muscles and ligaments surrounding them.
Sometimes there will be a need for assessments such as blood pressure monitoring, neurological tests (taking reflexes, testing muscle strength) or specific clinical orthopaedic (joint) tests. This varies depending on individual cases and your osteopath will explain the reasoning behind these situations as they arise. Osteopaths are trained to be safe before all else and we know when to look into things in a little more depth to make sure we're covering everything we need to.
Diagnosis

By now, your osteopath will have a good idea of what's going on . Although patients' presentations tend to evolve and change as they are treated, an initial "working" diagnosis will have been reached and this will be explained to you along with a treatment plan.
At this stage, if you have any questions, if you've not understood, if you'd like to see a diagram or a picture to better understand, that's absolutely fine. It's important that you feel in the know when it comes to your own body and health so your osteopath will do their best to make things simple and clear for you.
Treatment
When you are happy and if you want to continue you will receive treatment as part of your first session.
Treatments vary depending on your diagnosis and what you are comfortable with. Your osteopath will have an ideal treatment plan based on what they feel will be most effective for you. Most treatments involve some soft tissue work/stretching and joint mobilisations or adjustments, but you are in control and if there's something you don't like it is important that you say so. We will absolutely respect this. One of the beauties of osteopathy is the huge range of techniques and approaches, which mean there is often another way of getting the job done if need be.
Ongoing
Most people need a short course of treatments. This is hugely variable between individuals but a very rough ball park figure is 2-4 sessions to see initial settling of symptoms. More complex cases may be longer.
Beyond this, we'd ideally see you on a maintenance basis to keep things going. This can be anything from once every couple of months to a couple of times a year. Ideally we see you a little before you think you're in need as opposed to waiting for another catastrophe to hit - prevention is better than cure!
Legal Stuff!

The term osteopath became legally protected in 1993 and only those who have met strict guidelines and standards can become registered with the General Osteopathic Council (GOsC) and call themselves Osteopaths. All our osteopaths are GOsC registered.
GOsC registered osteopaths have completed at least a four-year full time course at a recognised college of osteopathy, completing over 2000 hours of clinic based experience and developing expertise in musculo-skeletal medicine based on osteopathic principles. They are also committed to a minimum of 30 hours of professional development annually in order to ensure their skills and knowledge are up-to-date.
If a warning light came on in your car would you ignore it, cover it up or seek professional advice? What about pain, your body's warning light? Call the professionals for some real solutions to pain.



 David McCabe
David McCabe
 Helen McCabe
Helen McCabe
 Kritika Bazgain
Kritika Bazgain




